Author: Nataliya Hanson, MS, OTR/L
Abstract
This case study presents a transgender man who was unaware of his pregnancy until presenting to the emergency room with complaints of watery discharge and abdominal pain. It explores the multifaceted barriers he faced in society, compounded by the challenges of becoming a birthing person. The patient’s real name has been withheld to protect confidentiality and will be referred to as JJ. This case brings to life the various domains that physical and occupational therapists assess and address to ensure patients remain safe and supported throughout their hospital stay. The study took place on the Mom and Baby Unit at Northwestern Medicine.
Background
From my initial chart review, the following is what I knew prior to meeting JJ. JJ is a 25-year-old African American individual with a female assignment at birth who now identifies as male and uses he/him pronouns. JJ has a history of Bipolar Disorder, Depression, Anxiety, PTSD, and dissociative identity disorder and has been unmedicated for the past two years. He recently ended a violent relationship that resulted in his partner’s incarceration, leading JJ to seek shelter in a domestic violence facility. During this time, JJ began exploring gender transition and had several appointments scheduled, but frequent ER visits for abdominal pain disrupted his plans. JJ felt dismissed by medical staff during these visits, as his symptoms were attributed to weight or past marijuana use. JJ has a history of drug misuse and weighs 461 pounds, with a BMI of 84. In a subsequent ER visit, JJ presented with abdominal pain and abnormal watery discharge, prompting an STD and cervical screening. Unexpectedly, JJ was found to be 33 weeks and 3 days pregnant: a discovery that took him by complete surprise. However, he confirmed that the sex was consensual. When asked about his home environment, JJ initially reported lacking housing or support and had been living at the shelter since the altercation with his ex-partner. At the time, he was unsure whether he wanted to keep the baby. JJ ultimately underwent an emergency cesarean section, losing 400 cc of blood during surgery. He gave birth to a baby boy who required minimal intervention: only a few steroid shots and supplemental oxygen on the first day. After meeting his son, JJ expressed excitement about parenthood and decided to keep the baby.
Patient Presentation
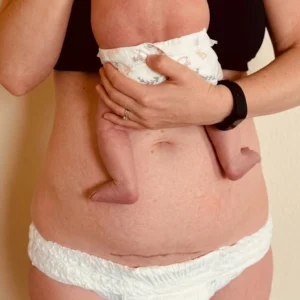
Upon meeting JJ, he was friendly and receptive. He welcomed both myself [the occupational therapist] and my physical therapy colleague into his room and was eager to learn about his postpartum recovery. Though JJ’s size was notable, he fit comfortably into a standard hospital bed. His baby boy was present in the room: an impressive sight for a 33-week-old infant!
JJ spoke candidly about estranged family relationships stemming from his last relationship. After a therapeutic discussion, he chose to contact family members. His mother, sister, and grandmother visited the same day, and JJ later reported that he would be moving in with his mother. However, he lacked basic necessities, such as a bed, due to his abrupt departure from his previous home. Although JJ expressed joy, underlying anxiety was apparent. I reassured him that we would address everything before discharge.
Differential Diagnosis
JJ underwent an emergency cesarean section. Research indicates that C-sections are associated with a 6–14 times greater risk of unplanned hysterectomy, which thankfully, JJ did not require during his procedure (National Academies of Sciences, Engineering, and Medicine, 2020; Leonard et al., 2019). However, risks such as pulmonary embolism (3.8x), stroke (5.8x), postpartum infection (5x), and chronic pain (12.3% incidence up to 10 months) are all significantly increased post-cesarean which I kept in mind with JJ. (National Academies of Sciences, Engineering, and Medicine, 2020; Leonard et al., 2019; Gunja et al., 2024). Additionally, as a person assigned female at birth and is African American, JJ is at heightened risk for cardiovascular disease, obesity-related complications, and pregnancy-associated conditions such as pre-eclampsia, embolism, and hemorrhage (Chinn et al., 2020). These predispositions, compounded by obesity and social determinants of health, underscored the need for thorough and anticipatory education from, not only the medical team, but from a rehabilitation perspective as well.
It is important to note here that 57% of postpartum deaths occur within six weeks, most commonly due to hemorrhage or infection (Tikkanen, 2020). These can often be identified by therapists during care if not caught by the primary medical team simply by doing vitals during mobility. Therapists understand what high blood pressure and low heart rate means or vice versa as we are skilled in monitoring vitals with every patient throughout the hospital no matter what floor they are on.
Rehab interventions
First, I typically start off with the abdominal binder for all my patients. Abdominal binders have been shown to reduce postoperative pain, improve physical function, and lower psychological distress after abdominal surgeries, including cesarean deliveries (Doganay et al., 2021; Elbohoty et al., 2021; Lukong et al., 2021). Unfortunately, we don’t have binders that fit JJ’s size. However, even if we did, this is a case where I actually wouldn’t give one out due to infection risk with increased sweat and moisture due to his pannus stomach. This is important to note, as individuals with obesity are at a significantly higher risk of postoperative infections due to impaired wound healing and reduced immune response (Waisbren et al., 2010). Another thing to remember is that JJ’s C-section was an emergency. Emergency cesarean sections are associated with an increased risk of postoperative infections compared to elective procedures due to the urgent nature of the surgery and less opportunity for preoperative preparation (Silver et al., 2015). Therefore, I taught JJ how to use a pillow combined with diaphragmatic breathing: a pillow to provide external support to the abdominal wall and diaphragmatic breathing techniques to facilitate pain control and decrease intra-abdominal pressure, thereby avoiding breath-holding and associated strain.
While JJ went for a two-minute walk test with the PT, which is the vitals check I mentioned earlier, I went along to educate on pre-eclampsia and hemorrhaging. Given JJ’s medical history, it was essential to cover these topics thoroughly, as understanding each condition and its potential presentation could be lifesaving if complications arise. Preeclampsia is most common 48 hours post-delivery and can occur up to the six-week mark. Signs and symptoms include high blood pressure (≥140/90 mm Hg), proteinuria (foamy urine), severe headaches, vision changes, swelling (especially in the face and hands), upper abdominal pain, nausea or vomiting, shortness of breath, and decreased urine output (American College of Obstetricians and Gynecologists, 2020). JJ’s mom was also following along behind us and reported that she had a blood pressure cuff at home and that they would use it.
The next education piece was mental health. JJ’s chart already told me that he had some chronic mental health difficulties. I provided JJ with education and had a full conversation about why it is important and how to receive assistance. After our conversation, JJ was willing and interested in managing his mental health with a psychiatrist. I educate every perinatal patient about mental health as baby blues turn into to Postpartum Depression (PPD) more quickly than people realize. 1 out of 5 to 7 women end up with PPD in some form (Postpartum Support International [PSI], 2022; Wisner et al., 2013). However, thinking about JJ specifically and his social determinates of health, I knew that racial discrimination and other environmental stressors contributes to the weathering of health for African Americans (Chinn et al., 2020).

Additionally, Black women are at increased risk for both short and prolonged sleep durations, obstructive sleep apnea, insomnia, and other indicators of poor sleep quality. Research indicates that, despite reporting lower sleep quality, Black women are less likely than women of other racial groups to disclose these disturbances to healthcare providers (Chinn et al., 2020). Given these findings, I prioritized a more in-depth conversation with JJ regarding sleep hygiene and barriers to restful sleep. During our discussion, JJ revealed that he did not have a bed to sleep on. Recognizing the physical effort required for JJ to perform a log roll to maintain abdominal precautions following surgery, I collaborated with the social work team to arrange for a hospital bed to be delivered to his home in order to promote safe recovery and improve rest quality.
I spoke to JJ about toileting at showering next, as Activities of Daily Living (ADL’s) are a big part of going back to life post-surgery and with a new depended. As an occupational therapist, I look at ADLs from a different lens. The most important one for me post-surgery is Metabolic Equivalents or MET levels. Most of the time, this population comes in independent in all aspects of life. Post surgery, people want to pick up where they left off, and most the time, the body isn’t ready for that. This is also the only surgery where the patient may go home with a dependent relaying mostly on them. For example, I tell my patients to try to avoid hot showers for the first couple weeks if they can. Activities with a MET level of approximately 4.9, such as walking at 4.0 mph, leisurely bicycling, gardening, or performing household tasks like washing windows, require moderate energy expenditure comparable to that of standing in a hot shower. These activities, while seemingly routine, can be physically demanding for postoperative or postpartum patients, underscoring the importance of careful assessment and guidance by therapists to ensure safe activity progression (Ainsworth et al., 2011). Therefore, I educate all my patients to attempt to avoid hot showers for a few weeks or at the very least use energy conservation strategies if they really enjoy hot showers.
These educational pieces were the ones I flagged as most important to go over with JJ. After these were covered, I also went over lactation, pelvic health therapy, positioning when caring for baby to prevent carpel tunnel, toileting, sit to stands with pain management, and reviewed all of JJ’s questions.
Outcomes
JJ and his newborn are doing well. He received a hospital bed, which has supported safe mobility at home. He also received comprehensive educational materials summarizing our discussions and reported referring to it. JJ attended a three-week follow-up appointment, and his medical status is stable: particularly regarding blood pressure management. JJ reported feeling well educated on his health which led to him being a confident first-time parent. With the discussion we had about mental health, he additionally found a provider and has started a medication regimen.
Plan of care
JJ’s plan of care includes follow-up visits at three, six, and twelve weeks with his OB. Due to his experience with therapy in the hospital setting, he came up with some money to hire an in-home occupational therapist for an initial session to optimize his home setup for recovery and infant care. Additionally, he found a psychologist that he is receiving medication prescriptions from as well as talking about his trauma with his ex-partner.
Reflection
Reflecting on this case, I thought about how the impact extended beyond JJ. I also educated the nursing staff, one of whom initially questioned the need for things such as a hospital bed, saying, “He can get up, he doesn’t need one.” While this seemed dismissive, I recognized it stemmed from a different clinical lens rather than malice. Nurses are trained differently than therapists and may not consider the same precautions and social factors. In her eyes, JJ was able to get out of bed therefore not needing a hospital bed. However, my lens showcased that JJ underwent a major procedure with a high BMI and lacked essential supports, and that he required me at his trunk to be able to get up with a log roll and maintain his precautions. Educating the staff throughout improved interprofessional understanding. JJ repeatedly voiced how supported and ready he felt to go home. He thanked me in particular for all the “real-life” tips as well as sitting down and discussing his social situation. This discussion motivated him to reach out to his family who then were happy to rekindle the bond. Additionally, his mother shared how much she wished she had received similar support during her own birthing experience. Hearing a parent say they feel prepared and unafraid: that is the power of holistic, compassionate rehabilitation care.
References
- Ainsworth, B. E., Haskell, W. L., Herrmann, S. D., Meckes, N., Bassett, D. R., Tudor-Locke, C., … & Leon, A. S. (2011). 2011 Compendium of Physical Activities: a second update of codes and MET values. Medicine and Science in Sports and Exercise, 43(8), 1575-1581. https://doi.org/10.1249/MSS.0b013e31821ece12
- American College of Obstetricians and Gynecologists. (2020). Preeclampsia and high blood pressure during pregnancy (FAQ034). https://www.acog.org/womens-health/faqs/preeclampsia-and-high-blood-pressure-during-pregnancy
- Chinn, J. J., Eisenberg, E., & Artis Dickerson, S. (2020). Maternal mortality in the United States: Research gaps, opportunities, and priorities. American Journal of Obstetrics & Gynecology, 223(4), 486–492. https://doi.org/10.1016/j.ajog.2020.06.014
- Doganay, G., Cavdar, I., & Ozsoy, S. A. (2021). The effect of abdominal binder use on postoperative pain, psychological distress, and physical function in cesarean delivery patients: A meta-analysis. Pain Medicine, 22(1), 173–182. https://doi.org/10.1093/pm/pnaa337
- Elbohoty, A. E., Salem, H. A., & Shady, N. W. (2021). Abdominal binder after cesarean delivery: Is it beneficial? A randomized controlled trial. Archives of Gynecology and Obstetrics, 303, 741–748. https://doi.org/10.1007/s00404-020-05784-z
- Gunja, M. Z., Karasawa, K., & Tikkanen, R. (2024). Maternal health inequity in the U.S.: A snapshot of race, place, and pregnancy outcomes. Commonwealth Fund. https://www.commonwealthfund.org/publications/issue-briefs/2024/apr/maternal-health-inequity-us
- Leonard, S. A., Main, E. K., & Carmichael, S. L. (2019). The contribution of maternal characteristics and cesarean delivery to an increasing trend of severe maternal morbidity. BMC Pregnancy and Childbirth, 19, Article 16. https://doi.org/10.1186/s12884-018-2144-5
- Lukong, C. S., El Nafaty, A. U., & Uba, F. A. (2021). The effect of abdominal binder on postoperative pain and recovery of physical function after open abdominal surgery. Nigerian Journal of Clinical Practice, 24(5), 707–713. https://doi.org/10.4103/njcp.njcp_403_19
- National Academies of Sciences, Engineering, and Medicine. (2020). Birth settings in America: Outcomes, quality, access, and choice. The National Academies Press. https://doi.org/10.17226/25636
- Postpartum Support International (PSI). (2022). Facts about postpartum depression and other perinatal mood disorders. https://www.postpartum.net/learn-more/
- Silver, R. M., Landon, M. B., Rouse, D. J., Leveno, K. J., Spong, C. Y., Thom, E. A., … & Varner, M. W. (2015). Maternal morbidity associated with multiple repeat cesarean deliveries. Obstetrics & Gynecology, 107(6), 1226-1232. https://doi.org/10.1097/AOG.0b013e3181f18c35
- Tikkanen, R., Gunja, M. Z., FitzGerald, M., & Zephyrin, L. (2020). Maternal mortality and maternity care in the United States compared to 10 other developed countries. Commonwealth Fund. https://www.commonwealthfund.org/publications/issue-briefs/2020/nov/maternal-mortality-maternity-care-us-compared-10-countries
- Waisbren, E., Rosen, H., Bader, A. M., Lipsitz, S. R., Rogers, S. O., & Eriksson, E. (2010). Percent body fat and prediction of surgical site infection. Journal of the American College of Surgeons, 210(4), 381–389. https://doi.org/10.1016/j.jamcollsurg.2009.12.036
- Wisner, K. L., Sit, D. K. Y., McShea, M. C., Rizzo, D. M., Zoretich, R. A., Hughes, C. L., … & Hanusa, B. H. (2013). Onset timing, thoughts of self-harm, and diagnoses in postpartum women with screen-positive depression findings. JAMA Psychiatry, 70(5), 490–498. https://doi.org/10.1001/jamapsychiatry.2013.87