Dr. Katelyn Lemond, PT, DPT, PCES
Core Connect Physical Therapy
Summary
A woman’s wellness, healing and experiences in pregnancy and postpartum are not linear. Bodily changes that affect posture, muscle strength, balance, and coordination are different for each woman, and a physical therapist can help peripartum women navigate these changes to improve their quality of life. However, often times there is little to no information given to her about what she may experience, how that may affect her journey, or how to address issues when they do arise. Back pain, stress urinary incontinence, diastasis recti abdominis, pelvic organ prolapse and pubic symphysis dysfunction are some of the most common issues that a woman may experience in both pregnancy and postpartum. When left unaddressed, women can have negative sequelae that may last for many years after they are done having children. Most women do not realize that there is help for these issues because they are not routinely offered rehab services. If more mothers were offered physical therapy visits during and immediately after delivery the negative consequences of pain, muscle weakness, posture imbalances, and incoordination would potentially be less prevalent. This is a case report of a 39-year-old mother who experienced diastasis recti, upper back/mid back pain, core weakness, and pubic symphysis dysfunction during, and after her third pregnancy. In this case report you will follow the journey of MS, a mother of three young children who endured months of hip, back and pubic pain during pregnancy. These pains led to reduced activity level, increased muscle weakness, poor posture, and difficulty caring for her young children. After a brief period of physical therapy during pregnancy, she decided to get follow-up help sooner than the standard six weeks postpartum guideline, and began physical therapy services in her home at three-and-a-half weeks postpartum.
Background
Diastasis Recti Abdominis (DRA) occurs when weakness of the anterior abdominal wall allows for separation along the rectus abdominis muscle in the midline of the abdomen1. This phenomenon is common in peripartum women. During pregnancy a woman has changes in hormone levels, a change in abdominal muscle length/position, and an increase in intraabdominal pressures due to the changing size of her uterus/position of the diaphragm. These combined changes are thought to contribute to the development of diastasis recti 2. Once a woman develops DRA, research indicates that it can become a long-term issue if not addressed, with a reported 82.6% prevalence rate in women one year postpartum in a study by Fei et al. 3. Risk factors for long-term postpartum DRA include higher BMI, diabetes, multi-gravida pregnancies and the width of the DRA being >2cm 2. If left untreated or mismanaged, diastasis recti abdominis has been linked with ongoing back pain, bladder/bowel dysfunction, painful intercourse, and pelvic/hip pain 4. Pelvic organ prolapse (POP) is another common adverse event that can occur after childbirth due to pelvic floor dysfunction and poor intraabdominal pressure management 5. Women who have had vaginal deliveries are at highest risk due to this delivery mode being known as the highest risk factor for having symptoms of POP 6. Difficulty managing intraabdominal pressure (IAP) after delivery due to muscle imbalances, muscle incoordination, and weakness is common in postpartum women. Pelvic organ prolapse can cause reduced quality of life for the women who experience it, and there are known complications to surgical interventions. Therefore, it is within reason for women to seek physical therapy to address management of intraabdominal pressure and core strength to address symptoms of diastasis recti and POP first 7.
Patient Presentation
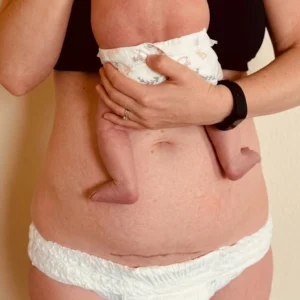
MS is a 39-year-old female who participated in an exercise class led by Dr. Katelyn Lemond, PT, DPT, PCES in February of 2025. The exercise class was a mix of cardiovascular endurance exercises and core exercises, safe for pregnant and postpartum women. During this class MS mentioned to Dr. Lemond that she had been seeing a physical therapist in an outpatient (OP) facility for pubic symphysis and hip pain. She was 31 weeks pregnant with her third baby at the time of the exercise class. During the core portion of the exercises, Dr. Lemond asked MS if she had ever been assessed for diastasis recti. MS told the physical therapist that she had, in fact, never been assessed for it. Dr. Lemond saw visible signs of a DRA, including doming at the midline of the rectus in an elevated supine position, as well as feeling a four-finger width separation in the same position. MS was receptive to basic education during and after the exercise class, and PT encouraged her to seek out physical therapy from an OB-educated PT for the remainder of her pregnancy if she wished, and definitely in the postpartum period. MS reportedly continued with PT at the OP facility for just one other treatment after the exercise class. She ended up delivering a baby girl vaginally in late March 2025, a couple of weeks before her due date. MS received Pitocin during her delivery, and delivered within two hours. Her mode of pain management was nitrous oxide only. She has a history of having a forced episiotomy with her first delivery that required forceps/vacuum assistance. Her second delivery was uncomplicated, as was her third. She reached out to Dr. Lemond after delivery with interest in starting postpartum physical therapy. At three-and-a-half weeks postpartum, she was evaluated in her own home by Dr. Lemond and her mobile physical therapy practice, Core Connect Physical Therapy.
Differential Diagnosis
MS had her at-home physical therapy evaluation in April 2025, with weekly follow-ups after to address her impairments. The results of her evaluation revealed impaired posture including forward head, rounded shoulders, thoracic spine stiffness, anterior pelvic tilt in standing, bilateral ribcage flare and a preference for shifting her pelvis to the left when standing. She had bilateral hip weakness, poor-to-fair diaphragmatic breathing techniques in various positions, three-finger width wide diastasis recti with one-third fingertip depth at the umbilicus, transverse abdominis weakness and incoordination, and pelvic floor weakness as observed from an external perspective. Her functional mobility was impaired, and she required reminders for using the log roll technique to get in and out of bed.

MS presented with tension in the upper abdominals, resulting in frequent breath holding and bearing down. Breath holding was observed with tasks such as sit to stand, getting up and down off the floor, and holding her newborn. She reported intermittent episodes of stress urinary incontinence, and briefly mentioned periods of feelings of heaviness in her vagina after activities like walking longer distances or carrying her 17-month-old toddler. At our third visit, she mentioned she felt she had a prolapse. She messaged her doctor, and was to see her the following week.
Rehab Interventions
On day one of examination, we began implementing gentle core movements and foundational breathing techniques. Exercises targeted proper breathing mechanics in various positions, transverse abdominis and pelvic floor activation and coordination in various positions, and gentle rotations of the midback for stretching.

Posture awareness was implemented by helping her understand a neutral pelvis position, as well as how to properly stack her ribs over her pelvis for exercise and during tasks like lifting. She was educated on the use of the abdominal binder in the short-term during more vigorous tasks, like pushing the stroller or lifting the car seat, in order to support her abdominal muscles and fascia.

Her vital signs were assessed before and after activities such as stair climbing to ensure proper cardiovascular response. We discussed the importance of proper core activation during activities like walking while pushing a stroller, and how breath coordination is valuable to reduce pressure down on the pelvic floor. On our third visit after MS mentioned symptoms of prolapse, we implemented new exercises for reducing pressure on the pelvic floor, as well as exercises to continue strengthening the pelvic floor. She was educated on strategies to use before and after her walks, or being on her feet for a prolonged period, to reduce the prolapse symptoms. She continued to struggle with coordination of breathing and deep core activation without cues, so we continued to work on those exercises in various positions like sidelying and hooklying to reduce her tendencies to hold her breath and bear down.
Outcomes
Measurements taken at the evaluation were her Diastasis Recti width and depth 8, manual muscle strength testing of the hips, thoracic rotation in a seated position, and observation and palpation of strength/coordination of the transverse abdominis and pelvic floor muscles. Also observed were her body mechanics with squatting, lifting, getting in and out of bed, going from sit to stand, holding her infant, and ascending/descending steps. MS responded well to verbal, visual and manual cues given while addressing muscle coordination and timing. She had difficulty with carryover to independent tasks, so the physical therapist attempted to modify exercises in the home exercise program to keep the client safe. Vital signs were taken before and after each visit to ensure proper cardiovascular response, and she was educated on typical and atypical responses 9. She was encouraged to obtain a pulse oximeter so that she could better monitor her heart rate response to more taxing exercises, like walking, since what we were doing in our sessions was more focused on breathing and gentle core movements.
Plan of Care
MS consistently followed-up with physical therapy for four weeks after her initial evaluation. In that timeframe, she was also seen by her delivering OB/GYN to assess her pelvic organ prolapse symptoms at her six-week follow-up. Her physical therapy plan of care included exercises to address breathing mechanics, posture awareness, thoracic mobility impairments, transverse abdominis and pelvic floor weaknesses, diastasis recti management, functional mobility adjustments and overall strengthening of her hips/legs. Dr. Lemond suggested a potential referral to a certified pelvic floor physical therapist for an internal exam of her pelvic floor function (specifically the function of the levator ani) if her POP symptoms were not improving after several weeks.10 Otherwise, the plan is to continue with postpartum physical therapy to address healing by learning strategies to manage IAP, increase her strength, improve her muscle coordination, and use proper lifting mechanics. In combination, these things have improved MS’s confidence to not only take care of her newborn and her other children, but also to advocate for herself when and if symptoms of other sequela arise.
Reflection
In-home physical therapy in the early postpartum phase of life can help improve a mother’s quality of life by offering support, reducing fear surrounding movement, encouraging proper body mechanics, and starting exercises for healing. With the incidence of things like diastasis recti and pelvic organ prolapse being high for the postpartum population, having a trained physical therapist provide services to women in their homes can reduce anxiety and fear that surrounds these topics.

Because MS was already seeing physical therapy when her symptoms of POP became more prominent, she was not as worried or fearful to address the issues head on. Mothers deserve to feel confident in their changing bodies, and physical therapy can be a great resource for providing hands-on training and education for safe mobility, proper exercise and healing after giving birth.
References
- Hall H, Sanjaghsaz H. Diastasis Recti Rehabilitation. PubMed. Published 2022. https://www.ncbi.nlm.nih.gov/books/NBK573063/
- Lin S, Lu J, Wang L, et al. Prevalence and risk factors of diastasis recti abdominis in the long-term postpartum: a cross-sectional study. Scientific Reports. 2024;14(1). doi:https://doi.org/10.1038/s41598-024-76974-x
- Radhakrishnan M, Ramamurthy K. Efficacy and Challenges in the Treatment of Diastasis Recti Abdominis-A Scoping Review on the Current Trends and Future Perspectives. Diagnostics (Basel). 2022;12(9):2044. Published 2022 Aug 24. doi:10.3390/diagnostics12092044
- Cleveland Clinic. Diastasis Recti (Abdominal Separation): Symptoms & Treatment. Cleveland Clinic. Published February 8, 2022. https://my.clevelandclinic.org/health/diseases/22346-diastasis-recti
- González-Timoneda A, Nerea Valles-Murcia, Esteban PM, et al. Prevalence and impact of pelvic floor dysfunctions on quality of life in women 5-10 years after their first vaginal or caesarian delivery. Heliyon. 2025;11(3):e42018-e42018. doi:https://doi.org/10.1016/j.heliyon.2025.e42018
- Hsu Y, Hitchcock R, Niederauer S, Nygaard IE, Shaw JM, Sheng X. Variables Affecting Intra-abdominal Pressure During Lifting in the Early Postpartum Period. Female Pelvic Med Reconstr Surg. 2018;24(4):287-291. doi:10.1097/SPV.0000000000000462
- Bø K, Hilde G, Stær-Jensen J, Siafarikas F, Tennfjord MK, Engh ME. Postpartum pelvic floor muscle training and pelvic organ prolapse: a randomized trial of primiparous women. American Journal of Obstetrics and Gynecology. 2015;212(1):38.e1-38.e7. doi:https://doi.org/10.1016/j.ajog.2014.06.049
- Diastasis Recti: What It Is and How to Fix It. Hospital for Special Surgery. https://www.hss.edu/article_diastasis-recti.asp
- Green LJ, Pullon R, Mackillop LH, et al. Postpartum-Specific Vital Sign Reference Ranges. Obstetrics & Gynecology. 2021;137(2):295-304. doi:https://doi.org/10.1097/aog.0000000000004239
- Dietz HP, Simpson JM. Levator trauma is associated with pelvic organ prolapse. BJOG. 2008;115(8):979-984. doi:10.1111/j.1471-0528.2008.01751.x
About the Author
Dr. Katelyn Lemond, PT, DPT is a mother of 3 boys, who saw the need for a change in rehab for postpartum women after the delivery of her own children. Recently she took action and began offering in-home pre/postnatal rehab services with her mobile therapy practice, Core Connect PT, in order to bridge the gap between post-delivery acute care and traditional rehab services that don’t begin until at least 6 weeks postpartum.